A New Normal For Hospital Care
(Posted on Tuesday, April 21, 2020)
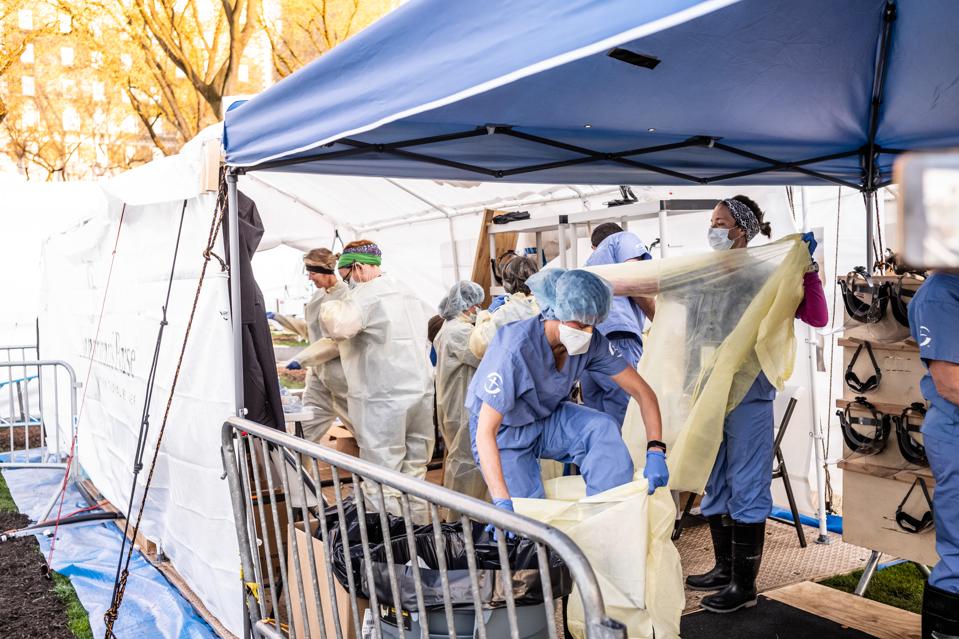
NEW YORK, NY April 08: Medical workers putting on PPEs at the beginning of their shift at the emergency field hospital run by Samaritan’s Purse and Mount Sinai Health System in Central Park on April 08, 2020 in New York, United States. (Photo by Misha Friedman/Getty Images)
GETTY IMAGES
Most hospitals and doctors offices are closed for business as usual. Many remain open for exceptional emergencies such as near fatal heart attacks and life threatening accidents. That leaves many of us without routine care or even care for serious chronic illness. For example, my follow up appointments for cancer care are cancelled indefinitely. Fortunately I am at very low risk for reoccurrence, but many people with serious chronic conditions are not so lucky.
The best estimate suggests that the combined toll of the pandemic on deaths not directly related to infection may be as great as the number of deaths form COVID-19 itself. That data comes from measurement of monthly excess deaths in Western European countries.
When we can return to hospitals and doctors offices for care, what will that care be like? Granted, telemedicine can fill part of the need, but certainly not all. We still need physical interactions with doctors. The Centers for Medicare and Medicaid Services recently offered guidance for what resuming medical care for non-COVID related illness should look like.
A few takeaways:
People should not return to hospitals for non-COVID care until the epidemic abates locally. Unfortunately, the criteria for abatement are not spelled out.
When hospitals reopen, non-COVID patients must be rigorously separated from COVID cases. That means separate facilities (entrances, waiting and examination rooms). That gives great advantage to those hospital systems that presciently invested in outpatient care facilities separate from full service hospitals. Here in New York, NYU Langone Health has created a network of many hundreds of such facilities in local communities distant from their hospitals.
Each patient must be screened for COVID before entering the hospital. That means a check for fever, cough, and other symptoms. Ideally it means each person should be subject to a rapid virus detection test (those that take five to 10 minutes). Once identified, COVID positive patients must be re-routed to specialized care facilities. Of course, this will not happen until we solve the testing issues.
All medical personnel must be regularly screened for infection. Whether screening should be daily or less frequently is not addressed. (The need for testing capabilities, highlighted again).
Patients and doctors should be required to wear protective masks at all times. Again, the guidelines are somewhat vague for what patient masks should be.
All facilities should be rigorously cleaned. Exactly how is also not specified.
Issues for care of children in foster care, prisoners, those mentally ill and with cognitive impairment or physical disabilities is not addressed in the guidelines. These are and will remain pressing issues.
Healthcare is an essential service for us all. Even after the pandemic, the experience of going to a hospital or even getting a checkup will not be what we remember it was for a long time.
Originally published on Forbes (April 21, 2020)

