Immunity To Covid-19 Infection May Fade Quickly
(Posted on Friday, June 19, 2020)
A new study published in Nature Medicine indicates that immunity to infection by SARS-CoV-2 may fade quickly, at least in people with no or moderate symptoms. The duration of protection from reinfection is a subject of intense interest both for convalescents returning to work and for vaccines.
The study focused primarily on two groups of 37 people who had been infected by SARS-CoV-2, as determined by repeated tests for viral RNA. One group never displayed clinical signs and symptoms of Covid-19 (asymptomatic). The symptomatic group all displayed mild symptoms of Covid-19 as determined by examinations by several physicians. The groups were matched for age and sex.
The first unexpected finding is that CAT-scans of the lung showed that two-thirds of those with no clinical signs of Covid-19 had what are called ground-glass opacity abnormalities typical of Covid-19 in at least one lung, and one-third showed ground-glass opacities in both lungs. In simple terms, SARS-CoV-2 is damaging the lungs of the majority who seem symptom-free. The long term health effects of such injuries may be apparent in later life.
A second somewhat unexpected finding is that the virus load upon initial detection was indistinguishable between the two infected groups. At least in the early stages of infection, the amount of virus detected in nasal swabs is not an indication of subsequent disease progression.
Viral RNA was detected in the nasal swabs of those infected for an average of 19 days in those with no clinical symptoms and 14 days for those who fell ill. Viral RNA was present as long a 45 days in one asymptotic individual and up to 22 days in a symptomatic patient. Detection of viral RNA may not be equivalent to the shedding of live virus. Nonetheless, the possibility is not excluded that transmission may extend past the usual quarantine period of 14 days. In recent times people in Northern China may be quarantined for up to 21 days post-exposure.
One purpose of the study was to measure the duration of the antibody response following infection in both the asymptomatic and symptomatic groups. The levels of Both IgG and IgM antibodies were measured 3-4 weeks post initial detection of infection and for two months thereafter.
The first surprise is that roughly 20 percent of people in both groups made no detectable IgG response to SARS-CoV-2. For IgM, the number was even lower. Between 30 to 40 percent of those infected had no detectable levels of IgM. That raises the question of how the virus is cleared (as it eventually was in all those studied) without robust antibody responses. We can speculate that may be due to a non-specific response from cells of the myeloid lineage or via a T-cell mediated immune response.
The levels of IgG neutralizing antibodies (as measured using a spike protein pseudotyped virus) were measured in both groups eight weeks after release from the hospital. The levels of IgG and neutralizing antibodies were significantly decreased in the majority of patients in both groups. The decrease in neutralizing antibodies was more pronounced in symptomatic as compared to asymptomatic patients.
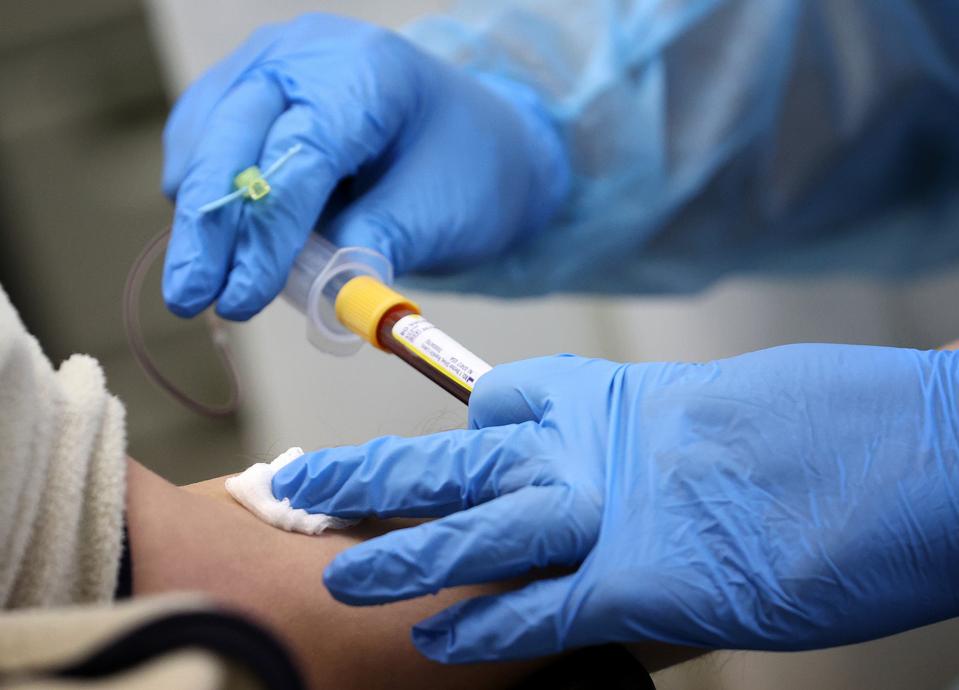
WASHINGTON, DC – JUNE 16: Residents have their blood drawn by registered nurse Barbara Davis for an antibody test for the coronavirus, also called a serology test, June 16, 2020 in Washington, DC. Serology tests are intended for persons who are not currently experiencing signs and symptoms of COVID-19, but want to know if they were previously exposed to the virus. (Photo by Win McNamee/Getty Images)
GETTY IMAGES
These are the most consequential results of this study. The finding that some people infected with SARS-CoV-2 infection do not make antibodies, added to the observation that neutralizing antibodies begin to drop noticeably a few weeks post-infection, raises the possibility that infection by SARS-CoV-2 does not establish long-lasting immunity, at least for those without symptoms or only mildly ill, more than 80% of all those infected by SARS-CoV-2
Patients with serious Covid-19 experience a cytokine storm, the equivalent of total body inflammation. Chemokines are proteins which play an important role in immune cell recruitment during inflammation. To explore this aspect of the disease further, the researchers compared the asymptomatic and symptomatic groups with a control group of 37 healthy, uninfected people, also matched by age and sex.
The levels of 18 chemokines were measured in all three groups. The levels of many (including TNF TRAIL, Mi-CSF, Gro-D. GCSF, and Il-6) were significantly increased in patients who had been infected versus the uninfected matched controls. There was no detectable difference in the level of chemokines those with asymptomatic infections and uninfected controls. This observation strongly implicates chemokines as a causative agent of observed Covid-19 symptoms. Recall that SARS-CoV-2 damaged the lungs of the majority of those who were asymptomatic.
The report also includes the curious observation that the levels of three proteins, stem cell factor, interleukin 3, and leukemia inhibitory factor were significantly higher in asymptomatic patients as compared to those with Covid-19 symptoms or were never infected. These are not inflammatory chemokines. As a group, these proteins promote blood cell formation and/or inhibit differentiation. Is this a hint of a protective response in those who never fall ill?
Undoubtedly this is the first of what will be a wealth of similar studies with much larger numbers as we have the opportunity to observe many more patients in the weeks and months following infection. What little we know now does raise concerns about the protective immune response to SARS-CoV-2 infection, concerns with profound implications for public policy and vaccination strategies.
This article originally appeared in Forbes (June 19, 2020).

